Children with motor disorders may have a significant delay in attaining motor milestones (such as being able to navigate stairs or tie their shoes), engage in repetitive and driven motions (such as rocking), or have physical or verbal tics. These habits, like those associated with other diseases, lead to impairment and unfavorable effects on one's physical health or social life.
Motor disorders are dysfunctions of the nervous system that cause involuntary actions or movements of the body or cannot be controlled by the individual. These conditions can result in either a lack of movement that was intentionally performed or an excessive amount of movement that was performed involuntarily. Motor disorders can manifest themselves in various ways, including tremors, jerks, twitches, spasms, contractions, or problems with gait. Motor disorders appear early in childhood and include difficulties with movement. The different motor disorders are distinguished by the kind of movement difficulties present and the persistence of symptoms. Seven motor disorders are mentioned in the Diagnostic Statistical Manual-5 (DSM-5): Developmental Coordination Disorder, Stereotypic Movement Disorder, Tourette's disorder, Persistent (chronic) vocal or motor tic disorder, Provisional tic disorder, Other Specified Tic Disorder, and Unspecified Tic Disorder.
Developmental coordination problems, stereotypic movement disorder, and tic disorders are the three primary groups that are included in the category of motor disorders.
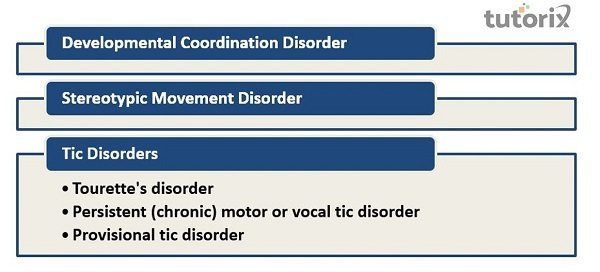
A developmental coordination disorder, motor skills condition, is characterized by substantial impairments in motor coordination as compared to the individual's age and intellectual capacity. A diagnosis of cerebral palsy or muscular dystrophy does not explain the inadequacies. In most cases, the presenting complaint will be a failure to fulfill certain developmental milestones. The inability of a newborn to hold up his or her head, reach, sit, or walk on time, as well as difficulties in eye-tracking, pincer-grasp, latching, suckling, and feeding, are all signs that point to the possibility of a developmental coordination disorder.
Stereotypic movement disorder is characterized by involuntary, purposeless, repetitive, and frequently rhythmic motor actions. These behaviors, including body rocking or hand flapping, interfere with developmentally appropriate everyday tasks. These behaviors occur in the earliest stages of development and are frequently linked to various other neurodevelopmental diseases, most notably profound intellectual disability. They might be self-harming, such as biting oneself, hitting one's skull, or slapping one's face.
Tics are sudden, purposeless, repetitive, nonrhythmic muscular actions or vocalizations. Even though they can imitate voluntary movement or speech, which can occasionally be inhibited, they are generally involuntary. Simple tics include facial expressions such as grimacing and jerking, coughing, eye blinking, and throat clearing. Tics that are more complicated include behaviors such as striking, touching, making obscene motions (copropraxia), and uttering obscenities (coprolalia).
The characteristics of an individual's tics—whether they be motor or vocal—are taken into consideration when classifying tic disorders.
Tourette's disorder: Tourette's disorder is characterized by multiple motor and one or more vocal tics at some point throughout the illness, although not necessarily simultaneously. Tics may increase or decrease in frequency over time, but they must be present for more than a year from the commencement of the first tic.
Persistent (chronic) motor or vocal tic disorder: It is a condition where single or numerous motor or vocal tics occur, but not both, that may wax and wane in frequency but last for more than a year following the commencement of the first tic. To properly diagnose chronic tic disorder, one must specify if the individual suffers "only from movement tics" or "only from verbal tics."
Provisional tic disorder: A single or multiple motors and vocal tic that has been present for less than a year after the commencement of the first tic is what defines someone as having provisional tic disorder. Tics can be either motor or verbal.
The requirements for either Tourette's or persistent tic disorder have not been satisfied since the disease must have been present for less than one year.
| Disorder | Description |
|---|---|
Developmental Coordination Disorder | Coordination of motor skills, both in development and execution, is far below age- and education-related expectations. Symptoms include clumsiness and motor skills that are delayed and incorrect. The onset occurs early in the course of development. |
Stereotypic movement disorder | Includes repeated, motivated, and aimless motor behaviours such as shaking, rocking, and self-hitting. The onset occurs early in the course of development. |
Tic Disorders
| Tics are abrupt, fast, repetitive, and nonrhythmic involuntary motions, noises, or phrases. More than one year of both verbal and motor tics, but not always simultaneously. The tics may fluctuate in frequency. onset occurs before age 18 One or multiple motor or verbal tics that occur several times a day or almost every day for over a year. Onset before age 18. Motor and verbal tics are incompatible with this diagnosis. One or more verbal and/or motor tics that have been present for less than one year. Onset before age 18. |
The underlying reasons for motor disorders are not well known. As with most psychological disorders, the data shows that several variables, including predisposition, learning, and environment, may contribute to the development of mental disorders.
Family studies indicated that tic disorders have genetic causes. Relatives of people with Tourette syndrome are 10 to 15% more likely to develop it or another tic disorder. Studies reveal that 25% of adolescents with stereotypic motor disorder have an afflicted relative. There are also chances of a family history of obsessive tendencies, mostly of counting rituals.
Learning factors may also contribute to motor disorder development and maintenance. Adolescents may be triggered to engage in tics or self-harm in stressful situations. After a tic or self-injury becomes habitual, similar triggers may elicit the same behavior. Adolescents with motor disorders have reported that tics or self-injury satisfy an unpleasant urge. Satisfying or reducing a need may strengthen the habit and raise the risk of repeating it.
Environmental variables can also cause motor disorders. Prenatal alcohol exposure can induce developmental coordination disorder and is associated with preterm and low-birth-weight children. Socially isolated children who tend to self-stimulate may develop stereotypic movements and repetitive self-injury. Traumatic brain injuries (e.g., concussion) can cause symptoms similar to stereotypic motor disorder.
There are currently no documented evidence-based practices for motor disorders, partly because the disorder can develop in multiple ways and because comorbid disorders and associated emotional challenges differ for each child. However, several studies have demonstrated that activity- and body-function-oriented strategies (such as physical and occupational therapy) are the most effective.
Therapies that attempt to strengthen motor function may use either a task- or process-oriented approach.
In a task-oriented approach, an observed motor problem (such as catching a ball) is identified, and the task is broken down into intervention steps that emphasize teaching and practicing the skill.
In a process-oriented approach, the therapist focuses on how children regulate their bodies and process sensory information. The hypothesis is that once the underlying mechanism producing the motor difficulty has been addressed, the associated motor abilities will likewise improve.
It includes:
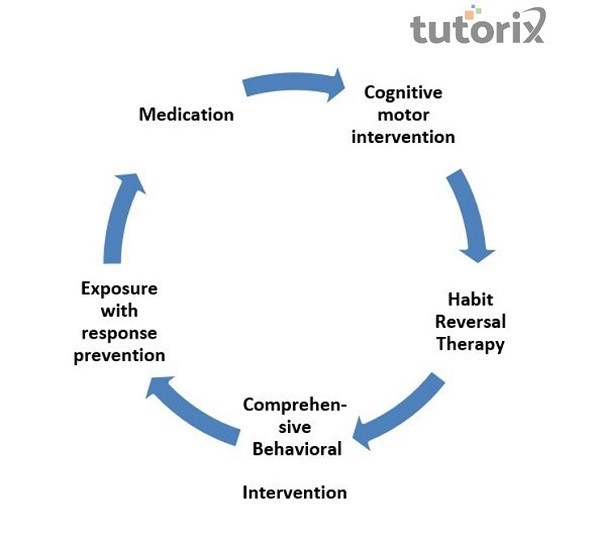
Cognitive motor intervention: Therapists curate a series of exercises for individuals to practice at home. Children are taught to organize, perform, and assess a movement, emphasizing emotional, motivational, and cognitive factors. Building self-confidence through positive reinforcement is an essential objective.
Habit Reversal Therapy (HRT): HRT teaches adolescents to recognize episodes of the habit, then the surroundings and internal feelings (e.g., recognizing stressful situations that trigger stereotypies). Once an adolescent can recognize feelings and events that trigger the habit, a competing response is taught.
Comprehensive Behavioral Intervention for Tics (C-BIT): C-BIT combines habit reversal, self-monitoring, tics education, and relaxing strategies. A therapist helps the child and family to understand tic patterns and triggers (CDC).
Exposure with response prevention (ERP): Consists of frequent and prolonged exposures to stimuli that cause discomfort and instructions to resist engaging in any action that reduces the discomfort.
Medication: Medicines are helpful in cases of moderate to severe tics that cause serious impairment in quality of life and in situations with co-occurring disorders.
Motor disorders are nervous system dysfunctions that result in involuntary or uncontrollable activities or movements of the body. The DSM-5 identifies seven motor disorders, including Developmental Coordination Disorder, Stereotypic Movement Disorder, Tourette's disorder, Persistent (chronic) vocal or motor tic disorder, Provisional tic disorder, Other Specified Tic Disorder, and Unspecified Tic Disorder. The fundamental causes of motor disorders remain unclear. As with most psychiatric problems, the research indicates that multiple factors, such as genetics, learning, and environment, may contribute to the onset of mental disorders. Some useful strategies, apart from medication, for the management of the disorders are Cognitive motor intervention, Habit Reversal Therapy (HRT), Comprehensive Behavioral Intervention for Tics (C-BIT), and Exposure with response prevention (ERP).